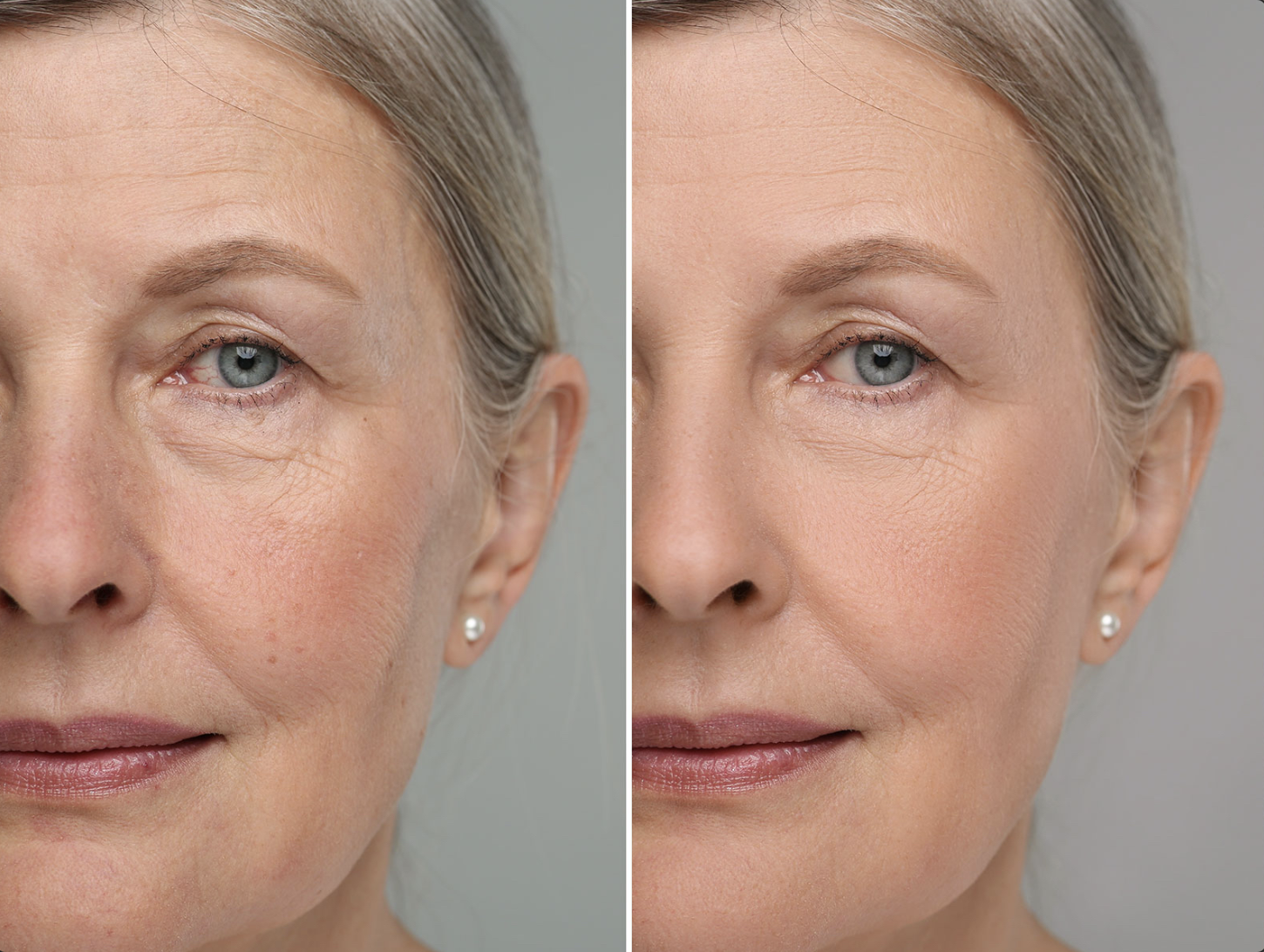
A “PDGF Facial” refers to an aesthetic treatment that harnesses the biological power of PDGF (Platelet-Derived Growth Factor) to stimulate skin renewal, collagen production, and tissue repair. In practice, it is often used in conjunction with other modalities (such as microneedling, lasers, or topical serums) to boost skin quality, reduce fine lines, improve texture and tone, and accelerate recovery from other skin procedures.
How it works — the science behind it
- PDGF is a naturally occurring protein growth-factor that platelets release in the body in response to injury or tissue damage. It helps recruit and stimulate cells (especially fibroblasts) that produce collagen and elastin, and it encourages angiogenesis (new-blood-vessel formation) and cell proliferation.
- In an aesthetic context, PDGF is used to activate or upgrade the skin’s own repair and renewal mechanisms. For example, after creating controlled micro-injuries (via microneedling) or laser treatments, applying or injecting PDGF helps the skin heal more robustly and regenerate more effectively.
- Some formulations are lab-engineered, pharmaceutical-grade PDGF (rather than a patient’s own blood-derived platelets), which allows for consistent dosing, no blood-draw required, and higher potency.
The Treatment Process
Depending on the clinic and specific protocol, a “PDGF Facial” might proceed somewhat like this:
- Consultation – The provider assesses your skin concerns (texture, tone, laxity, fine lines), medical history, and determines if PDGF is suitable.
- Preparation – The skin is cleansed, possibly numbed with a topical anesthetic (especially if microneedling or injections will be used).
- Primary modality – The provider may perform a skin-priming step such as:
- Microneedling (creating micro-channels).
- Laser or radio-frequency resurfacing (depending on skin condition).
- PDGF Application/Injection – The growth factor product is applied topically or injected into the skin. Some clinics use pre-filled syringes of pharmaceutical PDGF; others may use the patient’s own platelet derivates (less common in the true “facial” context).
- Aftercare – Post-treatment instructions may include limiting sun exposure, using gentle skincare, avoiding harsh exfoliants for some days, keeping skin hydrated, and scheduling follow-up. For example: avoid NSAIDs for a few days, use broad-spectrum SPF, avoid alcohol/smoking which impair healing.
- Results Timeline – Visible improvements in tone, texture, and firmness may appear over weeks or months as collagen builds and skin remodels. Some clinics recommend a series of treatments spaced 8-12 weeks apart for best outcomes.
What it treats & Benefits
The PDGF Facial is typically used for:
- Fine lines and wrinkles, especially around delicate areas (eyes, mouth).
- Skin laxity and loss of firmness/elasticity.
- Uneven texture, roughness, enlarged pores, dull tone.
- Scars or areas of skin damage (including from sun exposure or prior procedures) — by promoting tissue regeneration and improving skin architecture.
- It may also support post-procedure healing (after lasers, peels, microneedling) by reducing downtime and improving recovery quality.
Key benefits often cited:
- Stimulated collagen & elastin production → firmer, more youthful skin.
- Enhanced cell turnover and skin renewal leading to smoother texture.
- Improved vascularity (blood supply) which can improve skin glow and health.
- More consistent and predictable results (especially with lab-formulated PDGF) compared to older modalities like PRP (Platelet-Rich Plasma).
Risks, Downtime & Considerations
- The downtime is generally minimal, especially if only topical PDGF is used; you may experience mild redness, swelling, tenderness for a few hours or a couple days.
- If injections are used, there is slightly more risk (bruising, swelling, discomfort) although substantially less than more invasive procedures.
- Because PDGF is potent and biologically active, it must be administered by qualified professionals in a safe, sterile environment.
- Not all skin types or conditions are equally suited—for instance, active skin infections, open wounds, or certain autoimmune conditions might contraindicate use. (Some providers list pregnant or nursing women as not recommended for certain applications)
- Results depend on multiple factors: skin condition, the modality used (microneedling vs laser), number of sessions, aftercare, and how well one follows instructions.
- While PDGF shows promise, long-term aesthetic data is still accumulating; it may be considered as part of a broader skincare and aesthetic plan rather than a one-and-done “magic” solution.
Is it right for you?
You might be a good candidate if you:
- Are noticing early signs of aging (fine lines, mild laxity) and want a regenerative approach rather than only filler or toxin.
- Want to improve skin quality (texture, tone, glow) beyond what topical skincare alone can achieve.
- Are undergoing or have undergone a resurfacing/microneedling treatment and want to boost recovery and optimize results.
- Prefer minimally invasive treatments with modest downtime.
You might want to hold off or explore other options if you:
- Have active infection, uncontrolled skin conditions (e.g., significant dermatitis), or are pregnant/nursing (depending on clinic’s policy).
- Expect dramatic volume restoration (fillers may be more appropriate for deep volume loss).
- Are unable to commit to 1-3 sessions spaced out, or cannot adhere to aftercare (sun protection, avoiding certain medications, etc).
